Osteochondrosis is a chronic degenerative dystrophic disease that develops under the influence of many very disparate factors. Initially, the pathological changes occur in the nucleus pulposus (the inner contents of the intervertebral disc), and later, they spread to the annulus fibrosus (the outer shell of the disc) and other elements of the spinal motion segment (SDS). This can be a consequence of the body's natural aging process or it can occur against the background of injuries, increased loads on the spine and other causes. In any case, osteochondrosis is only the first stage of intervertebral disc destruction, and if left untreated, bulges and hernias form, which often require surgical removal.
The intervertebral disc is a cartilage formation that separates the vertebral bodies and acts as a shock absorber.
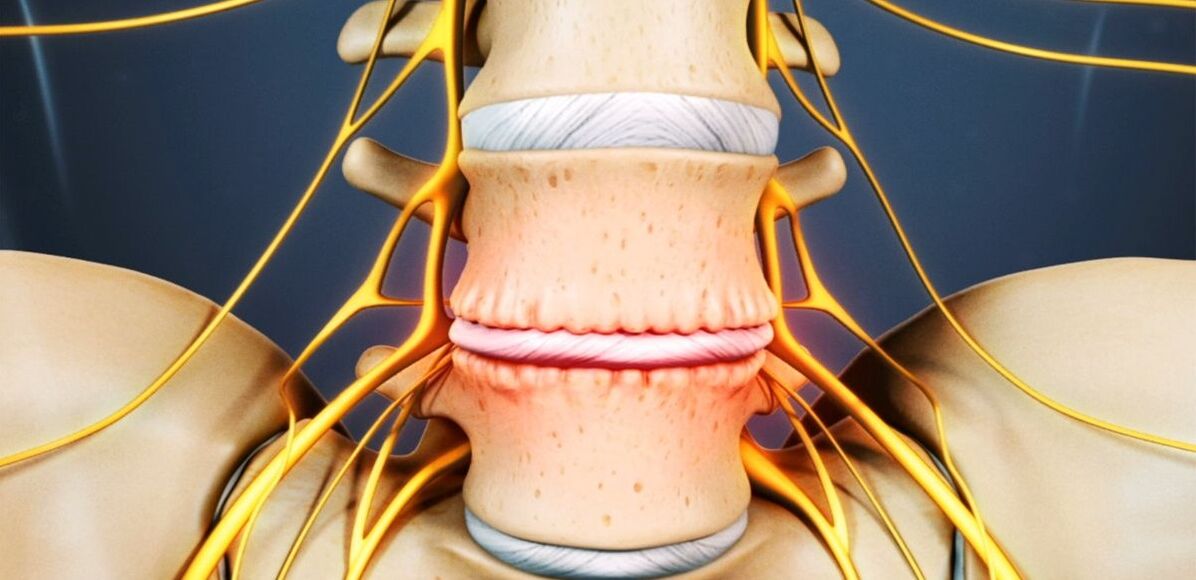
Osteochondrosis of the lumbar: what is it
From osteochondrosis suffers from 48 to 52% of people. And osteochondrosis of the lumbar spine is the most common. The disease can affect any one of the intervertebral discs in the lumbosacral spine, several of them, or even all of them. Most often L5-S1, L4-L5 disks suffer, less often L3-L4. The upper lumbar discs (L3-L2 and L2-L1) are affected much less frequently.
The prevalence of lumbar osteochondrosis is due to the fact that the greatest load in performing any physical work, especially lifting and carrying weights, walking, running, sitting, falls on the lumbar region. The lumbar spine consists of 5 vertebrae, which are much larger than the thoracic and cervical vertebrae. Thus, the intervertebral discs that separate them are larger in size. Normally, the lumbar region has a slight anterior curvature (physiological lordosis). It is the last mobile part of the spine and is adjacent to the fixed sacrum, so most often they talk about lumbosacral osteochondrosis.
If previously osteochondrosis was considered an age-related disease, today its first manifestations can already be observed at 15-19 years of age. Among the age of thirty, already 1. 1% of people suffer from severe symptoms of degenerative-dystrophic changes in the intervertebral discs. And in representatives of the more advanced age group (from 59 years old), the clinical manifestations of the disease are already present in 82. 5%. At the same time, the incidence of the pathology continues to grow steadily, which is largely due not only to the increase in the average age of the country's population, but also to changes in lifestyle that are not for the better.
reasons for development
Today, there is still no consensus on the etiology of degenerative diseases of the spine. However, the main theory of its development is involutionary. According to her, osteochondrosis is a consequence of previous damage to the intervertebral disc and bone structures of the spine, in addition to the occurrence of inflammatory and other processes. The theory suggests that degenerative changes are genetically predetermined and, in fact, inevitable. And its clinical manifestation, especially in young and middle-aged people, is due to the influence of several endogenous and exogenous factors.
Thus, the development of osteochondrosis of the lumbar spine is facilitated by:
- heavy physical work, especially associated with heavy lifting;
- sedentary, sedentary lifestyle;
- any back injury, including bruising;
- overweight;
- metabolic disorders;
- posture violations, deformation of the spine;
- flat feet and other foot pathologies;
- pregnancy, especially multiple pregnancy.

pathogenesis
Regardless of the causes, intervertebral disc degeneration occurs when the intensity of catabolism processes (cleavage and oxidation of molecules) of matrix proteins begins to exceed the rate of their formation. One of the key points in this process is the malnutrition of the intervertebral discs.
As they, like most adult cartilages, do not have a direct blood supply, as they lack blood vessels, the supply of nutrients to them and the removal of metabolic products occurs by diffusion with sequential compression and relaxation of the disc during movement. The main structure that powers the disk are the end plates located on its top and bottom surfaces.
By themselves, the endplates are a bilayer formed by cartilage cells and bone tissue. Thus, the cartilaginous side are adjacent to the disc, and the bone - to the vertebral bodies. They are distinguished by sufficiently good permeability, which ensures the exchange of substances between the cells, the intercellular substance of the disc and the blood vessels passing through the vertebral bodies. Over the years, especially with the negative impact of external and internal factors, the structure of the endplates changes and their blood supply decreases, which leads to a decrease in the intensity of metabolism in the intervertebral disc. As a result, its ability to produce new matrix is reduced, which leads to a progressive decrease in its density with age.
At the molecular level, this is accompanied by:
- a decrease in the rate of diffusion of nutrients and metabolic products;
- decreased cell viability;
- accumulation of cellular breakdown products and altered matrix molecules;
- decreased production of proteoglycans (high molecular weight compounds responsible for the formation of new cartilaginous cells and which are the main sources of synthesis of chondroitin sulfates);
- Collagen scaffolding damage.
Possible consequences
As a result of the ongoing changes, the intervertebral disc becomes dehydrated and the nucleus pulposus loses its ability to properly distribute the loads that fall on it. Therefore, the pressure within the disc becomes uneven and therefore the annulus fibrosus in various places is overloaded and compressed. As this happens with every movement a person makes, the ring is regularly subjected to mechanical pressure. This leads to adverse changes in it.
In addition, a decrease in disc height and elasticity often leads to compensatory changes in adjacent vertebral bodies. Bone growths called osteophytes form on their surfaces. They tend to increase in size over time and even merge together, excluding the possibility of movement in the affected PDS.
Due to the fact that malnutrition causes damage to the collagen skeleton, under the influence of pressure from the nucleus pulposus at certain points, the normal structure of the fibers that form the annulus fibrosus is disrupted. In the absence of intervention, this ends up leading to cracks and breaks in them. Gradually, more and more fibers of the annulus fibrosus at the site of application of pressure are torn, which leads to their protrusion. This is especially facilitated by the increased loads on the column. And since the lower back takes the main load during movement and any physical activity, it suffers more often.
The protrusion of the intervertebral disc without the final rupture of the annulus fibrosus and with the size of its base greater than the protruding part is called the protrusion. With its complete rupture in one place or another, an intervertebral hernia is diagnosed.
With the destruction of part of the fibers of the annulus fibrosus, the pressure on the disc gradually decreases, which leads to a decrease in tension and in the fibers themselves. This leads to a violation of its fixation and, as a result, to pathological mobility of the affected spinal movement segment.
The vertebral motor segment (SMS) is a structural and functional unit of the spine formed by the intervertebral disc, adjacent vertebral bodies, their facet joints, ligaments and muscles attached to these bony structures.
The normal operation of the column is only possible with the correct operation of the PDS.
Symptoms of Osteochondrosis of the Lumbar Spine
The disease may be asymptomatic for a long time, and then begin to manifest as mild discomfort in the lower back, gradually gaining strength. But in some cases, osteochondrosis of the lumbar begins acutely, immediately causing a powerful pain syndrome. In most cases, signs of pathology first appear after 35 years.
Back pain is the main symptom of the disease. It can be of different character and be painful and dull, and acute, constant or episodic. But basically for the pathology, especially in the early stages of development, the alternation of periods of exacerbation and remission is characteristic, and both hypothermia or the lifting of a heavy object, as well as a sudden and unsuccessful movement can provoke another deterioration of well-being. .
The pain is often accompanied by a feeling of numbness and tension in the back muscles. They are made worse by physical exertion, sudden movements, heavy lifting, bending over, and even coughing and sneezing.
If, due to instability of the vertebral bodies, the nerve root extending from the spinal cord is pinched by one or another anatomical structure, this will lead to the development of appropriate neurological disorders. Its main manifestations are:
- shooting, severe pain radiating to the sacrum, buttocks, lower limbs or perineum;
- sensitivity disorders of varying severity;
- mobility restrictions, lameness;
- weakness in the muscles innervated by the pinched nerve.
In the lumbar spine, the spinal cord ends at the level of 1-2 vertebrae and passes into the so-called cauda equina, formed by an accumulation of spinal roots. In addition, each of them is responsible not only for the innervation of muscles, but also for specific organs of the small pelvis, so prolonged compression can cause disturbances in the work of the corresponding organ. This can lead to the development of impotence, infertility, gynecological diseases, hemorrhoids and other disorders.
The clinical picture of osteochondrosis of the lumbar spine, especially with a long course and the occurrence of compression of the spinal roots, depends a lot on the level of the lesion, that is, which specific disc has suffered degenerative-dystrophic changes.
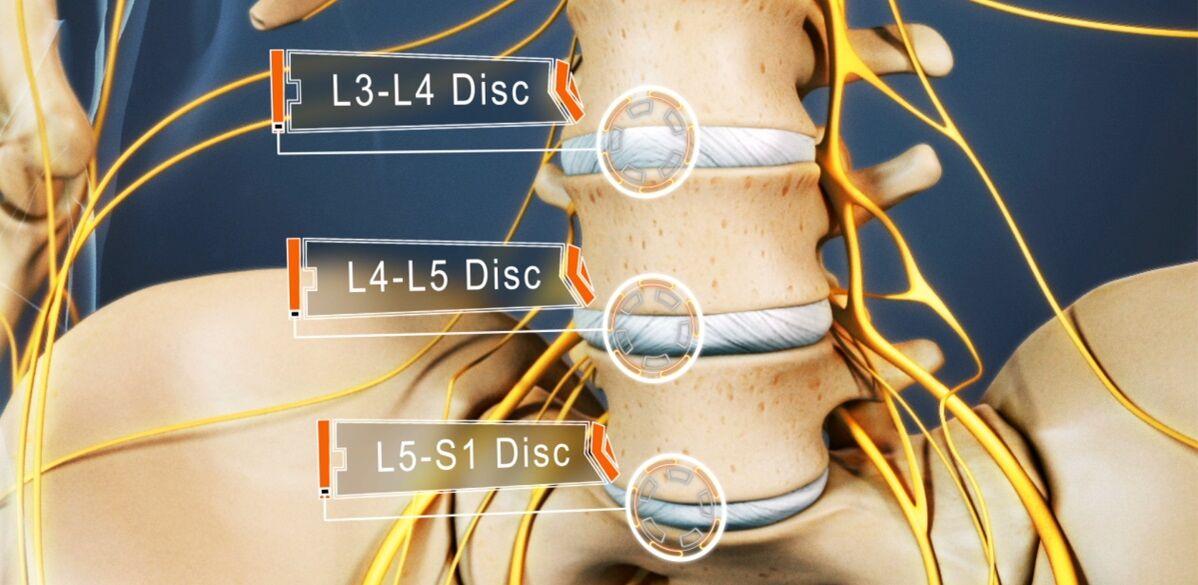
- L3-L4 disc defeat - pain is given to the antero-inner parts of the inner thigh, lower leg and ankle. This is accompanied by a decrease in the sensitivity of the anterior surface of the thigh, a decrease in gravity or loss of knee motion, as well as a decrease in quadriceps muscle strength.
- L4-L5 disc defeat - pain is given from the upper part of the buttocks to the outer parts of the thigh and lower leg. Less commonly, this is accompanied by spreading pain to the back of the feet, including 1-3 toes. In these areas, there is decreased sensitivity and muscle weakness. Sometimes hypotrophy and incomplete extension of the big toe develops.
- L5-S1 Disc Damage - Pain starts in the mid-buttocks and goes down to the heel along the posterior or posterior surface of the thigh and lower leg and can capture the outer edge of the foot like 4-5 toes. In these areas of the lower extremities, there is a decrease in sensation, and the gastrocnemius and gluteus maximus often decrease in size, which is accompanied by their weakness. If the spinal root that passes at the level of this PDS is affected, a decrease or loss of the Achilles and plantar reflexes may be observed.
L1-L2 and L2-L3 disks are rarely affected.
The pain that accompanies the disease restricts a person and significantly reduces the quality of his life. As they persist for a long time and recur regularly, if not constantly present, this cannot but affect the psycho-emotional state. As a result, more than half of patients show signs of chronic emotional stress, depressive disorders, etc.
Diagnosis
If there are signs of osteochondrosis of the lumbar spine, you should contact a neurologist or vertebrologist. First of all, the doctor collects an anamnesis, which consists of clarifying the nature of the complaints, the characteristics of the pain, the conditions for its occurrence and reduction, the characteristics of a person's professional life, etc.
The second stage of diagnosis, performed as part of the first consultation with a doctor, is a physical examination. During it, the doctor assesses the condition of the skin, posture, the depth of the physiological curves of the spine, the presence of its curvature, etc. they are often painful and excessively tense, which is a reflex reaction of the body to inflammation and discogenic pain.
Based on the data obtained during the examination and questioning of the patient, the neurologist may suspect the presence of osteochondrosis of the lumbar spine. But in order to exclude possible concomitant pathologies, as well as confirm the diagnosis and accurately determine the level of damage, the severity of degenerative-dystrophic changes in the intervertebral disc and the involvement of bony structures, laboratory and instrumental diagnostic methods are required.

laboratory diagnosis
Analyzes of various types are not decisive in the diagnosis of osteochondrosis of the lumbar spine. They are more aimed at assessing the degree of the inflammatory process and detecting concomitant disorders.
Thus, they can be assigned:
- YOU ACCEPTED;
- THE AM;
- blood test for sugar level;
- blood chemistry.
Instrumental diagnostics
All patients with suspected lumbar spine osteochondrosis have:
- x-ray of the lumbar spine in two projections - allows to determine the structure of bone structures, detect anomalies, osteophytes formed, changes in facet joints, etc. ;
- CT - allows detecting changes in bone structures at earlier stages of development than radiographs, in addition to identifying indirect signs of osteochondrosis;
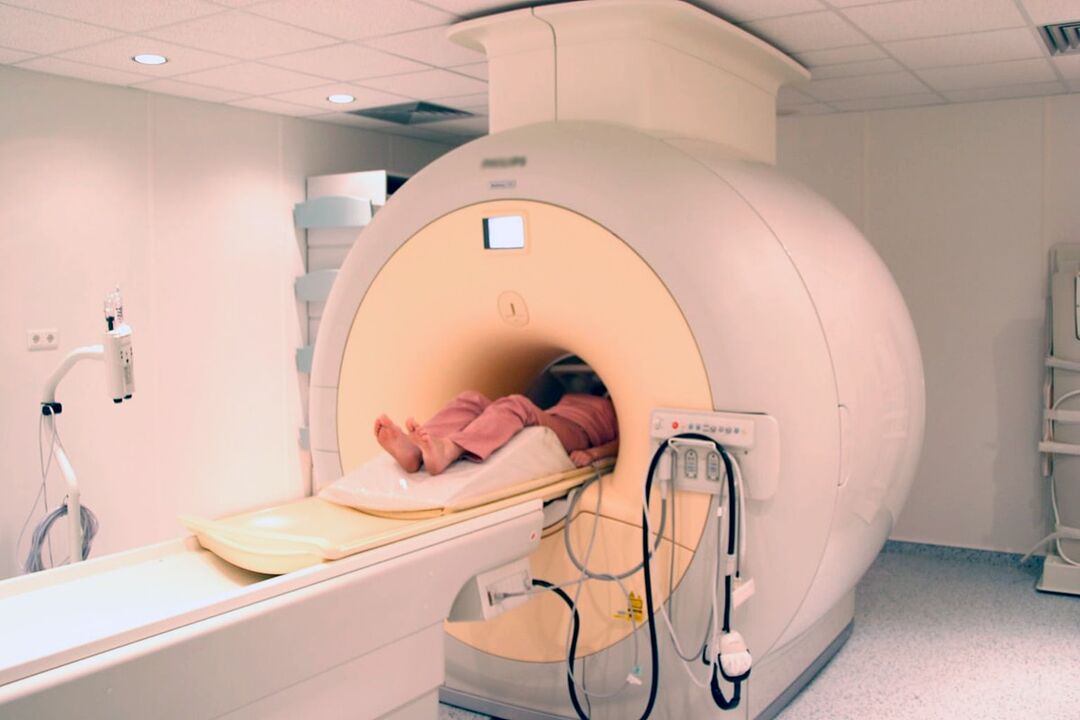
- MRI is the best method for diagnosing pathological changes in cartilage formations and other soft tissue structures, which allows you to detect the smallest changes in intervertebral discs, ligaments, blood vessels and spinal cord and accurately assess their severity and potential risks.
In addition, it can be recommended:
- densitometry - a method for determining bone density, which makes it possible to diagnose osteoporosis, which is especially common in the elderly;
- myelography - allows assessing the state of the CSF pathways of the spinal cord and the degree of damage to the protruding disc, which is especially important in the presence of an already formed intervertebral hernia of the lumbar spine.
Treatment of lumbar osteochondrosis
When diagnosing osteochondrosis, as a rule, initially all patients receive conservative therapy, provided that there is no pronounced and progressive neurological deficit. But your character is selected strictly individually.
As the disease is chronic and the regenerative capacities of the intervertebral discs are extremely limited, especially with pronounced degenerative-dystrophic changes, the main goals of therapy are to stop its progression and eliminate the symptoms that bother the patient. Therefore, treatment is always complex and includes:
- drug therapy;
- manual therapy;
- physiotherapy;
- exercise therapy.
In the acute period, patients are shown to limit physical activity or even adhere to bed rest for 1-2 days. This will help relax the muscles and reduce pressure inside the disc. If you need to sit, walk, or do physical work for a long time, wear a stabilizing lumbar corset.

After the end of the acute period and during the remission of the disease, on the contrary, it is important to move as much as possible, but with caution and excluding increased stress on the lower back. Patients will need to acquire the skills to sit properly, lift objects off the floor, carry heavy loads, as these all affect the course of the pathology. It is important to avoid leaning and sudden movements, lifting something off the floor or low surfaces, after bending your knees and not bending down. You should only sit with your back straight in a chair that supports your back. Also, during sedentary work, it is important to regularly take breaks for a short workout. It is important to avoid falls, jumps, fast runs and hypothermia.
In osteochondrosis, it is important to maintain body weight within the ideal limits, and for obesity, diet and physical exercises appropriate to the patient's condition are indicated, as excess weight generates an increased load on the lumbar region and causes a faster progression of pathological changes in the discs.
On average, conservative therapy is usually designed for 1-3 months, although it may last longer. But even after completing the main course prescribed by the doctor, it will be necessary to continue taking various medications, exercise therapy and following lifestyle recommendations.
medical therapy
The main components of drug therapy are drugs selected individually from the NSAID group. When choosing them, the doctor takes into account not only the severity of the pain syndrome and the course of the inflammatory process, but also the nature of concomitant diseases, especially of the digestive tract, since NSAIDs with prolonged use can adversely affect the state of their mucous membranes and provoke an exacerbation of various pathologies of the digestive system.
It is necessary to use NSAIDs for acute pain in the lower back and immediately after its occurrence. Preferably in 1-2 days. Depending on the severity of the patient's condition, they can be administered intramuscularly, in the form of rectal suppositories, local agents, and in oral form. The duration of admission must not exceed 2 weeks. In the future, an individually selected drug is taken on demand, but trying to avoid frequent use.
Recently, more preference is given to drugs, as an active ingredient, which include selective inhibitors of cyclooxygenase-2.
In addition, patients are prescribed drugs from the following groups:
- muscle relaxants - help to relax overly tense muscles and thus reduce back pain;
- chondroprotectors - improve the course of metabolic processes in the intervertebral disc (especially effective when started in the early stages of development of lumbar osteochondrosis);
- B vitamins - contribute to the improvement of nerve conduction;
- antidepressants and anxiolytics - used for long-term osteochondrosis, which has led to depression, chronic fatigue, and other psychological disorders.
With very intense pain, mainly of neurological origin, therapeutic blocks are performed. They involve the introduction of anesthetics in combination with corticosteroids at points close to the pinched nerve, which leads to rapid elimination of pain. But the procedure can only be performed in a medical institution by specially trained healthcare professionals, as it is associated with a risk of complications.
Manual therapy
Manual therapy allows not only to improve the quality of blood circulation in the area of influence, but also to significantly reduce the severity and duration of pain in osteochondrosis. Effectively relieves muscle tension and allows to eliminate functional blocks, which significantly increases mobility in the affected SMS.
Furthermore, through well-conducted manual therapy, it is possible not only to increase the distance between the vertebrae, to return them to their anatomically correct position, but also to release the compressed nerve roots. As a result, the pain is quickly eliminated and the neurological disorders disappear. It also reduces the likelihood of complications and disturbances in the work of internal organs.
Additional positive properties of manual therapy are improving mood, strengthening immunity, activating the body's natural recovery mechanisms and increasing efficiency. Usually after the 1st session there is a noticeable improvement in well-being, and in the future the effect becomes more pronounced. As a rule, the course consists of 8-15 sessions, and it is important to complete it to the end, even with the complete normalization of well-being.
Physiotherapy
After the decrease of acute inflammation, courses of physiotherapeutic procedures are indicated, which not only help to reduce pain, but also improve microcirculation, nutrition and the course of repair processes in the area of degenerative dystrophic changes. Most often, patients are prescribed:
- electrophoresis with drug introduction;
- electrical neurostimulation;
- ultrasound therapy;
- laser therapy;
- magnetotherapy;
- UHF.
Which specific methods of physiotherapy will give the best effect, the frequency of their implementation, the duration of the course and the possibility of combining with other types of exposure are determined individually for each patient.

Traction therapy gives very good results in osteochondrosis of the lumbar spine. Thanks to this, it is possible to obtain an increase in the distance between the vertebral bodies, which instantly reduces the load on the affected discs. After the session, to consolidate the results, the patient must wear an orthopedic corset.
exercise therapy
After the elimination of acute pain, the treatment program is necessarily supplemented with exercise therapy. Its main tasks are to lengthen the spine and relax the spasmodic muscles of the lower back. In addition, therapeutic exercises help strengthen the muscular corset, create reliable support for the spine, and improve posture. In the course of this, blood circulation is inevitably activated and metabolic processes are improved, which has a beneficial effect on disc nutrition.
For each patient, a set of exercises is selected individually according to the degree of degenerative-dystrophic changes, the patient's level of physical development, the nature of concomitant disorders, age and other factors. Initially, it is recommended to study under the guidance of an experienced exercise therapy instructor.
It is recommended that all patients with degenerative changes in the spine visit the pool 2-3 times a week, as swimming lessons minimize the load on the spine, but allow you to effectively strengthen the back muscles.
Thus, osteochondrosis of the lumbar spine is one of the most common diseases. At the same time, it is able to deprive a person of the ability to work for a long time and even lead to disability due to the development of complications. Therefore, it is important not to ignore the first symptoms of the disease, when it is easier to deal with it. With the onset of pain, and even more numbness, limited mobility, back pain, you need to contact a neurologist as soon as possible, take the necessary examination and start treatment. In this case, it will be possible to stop the pathological process and return to a normal and full life, without pain and significant restrictions.

























